Regenerative Medicine in Veterinary Practice: Perceptions, Experience, and Outlook

Regenerative medicine is evolving rapidly in humans and pets, and the first FDA-approved mesenchymal stromal cell (MSC) therapy in veterinary medicine is anticipated in 2026, targeting refractory feline chronic gingivostomatitis. To learn how veterinary professionals are navigating the evolving regenerative medicine landscape, Gallant collaborated with the American Animal Hospital Association (AAHA) to conduct this survey.
Many veterinarians and veterinary technicians maintain early impressions of MSC therapy based on experiences with autologous (tissue harvested from patient), point-of-care preparations that may differ substantially from standardized allogeneic (tissue harvested from healthy donor) products. Capturing contemporary practitioner experience is critical to understanding how MSC therapies are applied in everyday practice, how newer products are perceived relative to earlier approaches, and where gaps remain between published evidence and clinical implementation.
This descriptive cross-sectional study was initiated by Gallant and administered by the American Animal Hospital Association (AAHA). It employed an online survey approach, wherein participants received a hyperlink to access the survey generated by and hosted on Qualtrics XM software. The survey was a structured exploratory survey, distributed to AAHA’s members. The survey included an introductory section with background information on regenerative medicine and 34 close-ended and 4 open-ended questions.
This survey was designed to assess satisfaction with current treatment options for chronic inflammatory conditions, explore familiarity and confidence with regenerative modalities, and document real‑world usage patterns across canine and feline patients. It also sought to identify perceived advantages, concerns, and unmet needs related to emerging regenerative products, particularly donor‑derived, off‑the‑shelf stem cell therapies, and understand expectations for their future role in veterinary medicine.
Data collection took place over 17 days in November 2025. As an incentive for participation, respondents were entered into a raffle to win one of ten $200 Amazon gift cards. A total of 34,958 suspected eligible respondents were invited to participate, yielding 1,095 (3%) qualified respondents based on identifying veterinarians or veterinary technicians working in small animal or mixed animal practices. The number of respondents to each question varied according to respondent ability to answer each question. Survey responses are summarized below.
Participants
Veterinarians comprised 70.4% and veterinary technicians 29.6% of the total population. Most respondents worked in companion animal practices (91.2%), followed by mixed animal (7.6%) and feline-only practices (1.2%). The average age of respondents was 48 years old, (veterinarians averaged 50 years, veterinary technicians averaged 41 years). The largest age group was 35–44 (30.7%), followed by 45–54 (24.8%), 25–34 (17.6%), 55–64 (16.6%), over 65 (9.6%) and 18-24 (0.6%).
Current Satisfaction with Treatment Options for Chronic Inflammatory Conditions
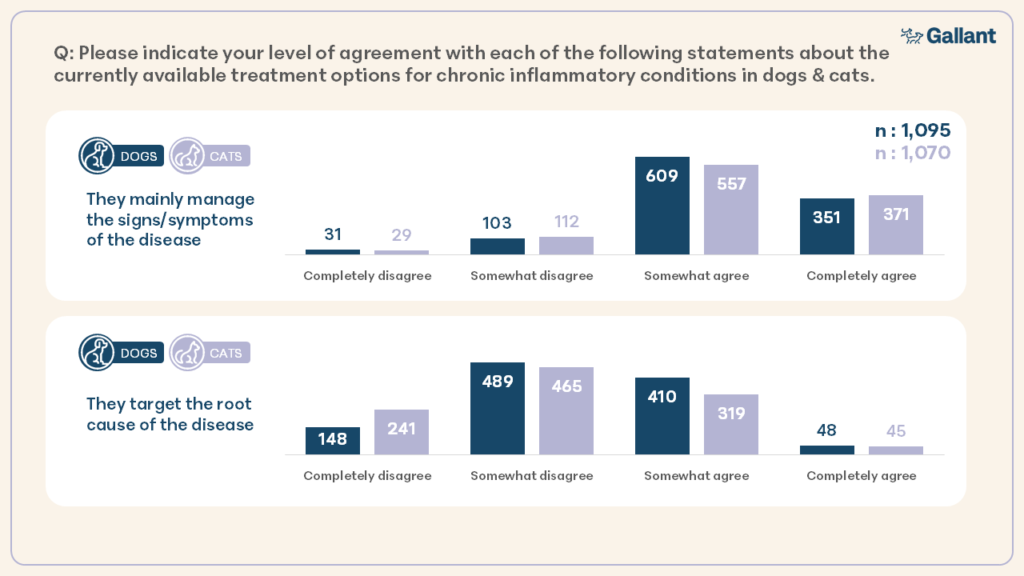
When asked their level of agreement with statements about the effectiveness of currently available treatment options (Figure 1), 87.8% and 86.8% respondents felt that current treatments primarily manage symptoms in dogs and cats respectively. 41.8% and 34% of respondents believed current therapies target the root cause of disease in dogs and cats respectively.
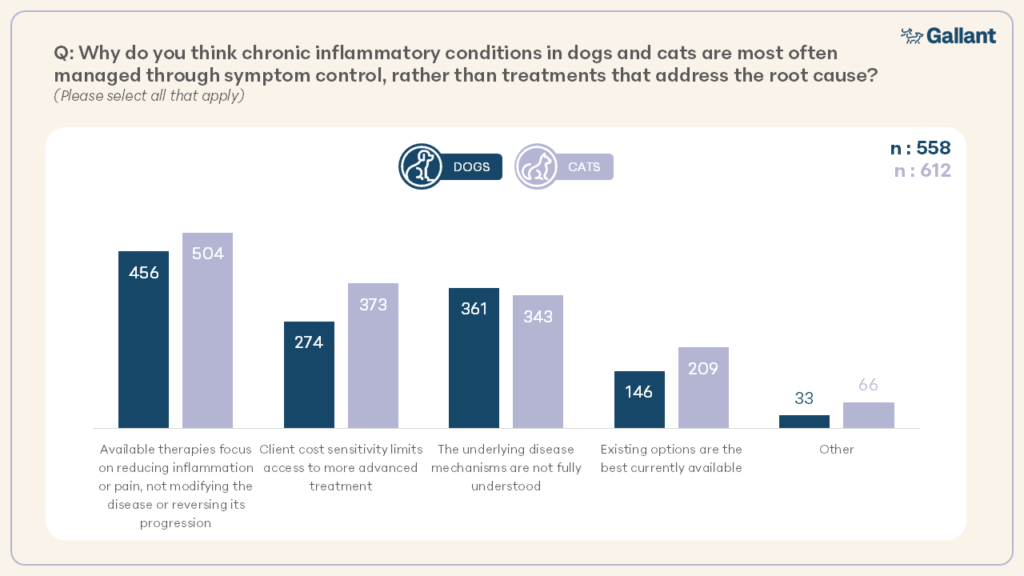
Among those who agreed that current treatments mainly manage symptoms and don’t target the root cause (Figure 2), the most common reasons why were that available therapies focus on reducing inflammation or pain without modifying the disease (81.7% dogs, 82.4% cats), client cost sensitivity limits access to more advanced treatment (66.1% dogs, 60.9% cats), and the underlying disease mechanisms are not fully understood (49.1% dogs, 56% cats).
Among those who selected “other,” feline specific responses highlighted limited feline-specific research, challenges with medication administration and compliance, fewer treatment options due to feline physiology, and lower owner investment in care in cats compared to dogs.
When asked to describe the current standard of care for managing chronic inflammatory conditions in their own words, open ended responses were categorized and totaled from 1040 comments in 1016 respondents regarding dogs and 1066 comments in 974 respondents regarding cats (Figure 3).
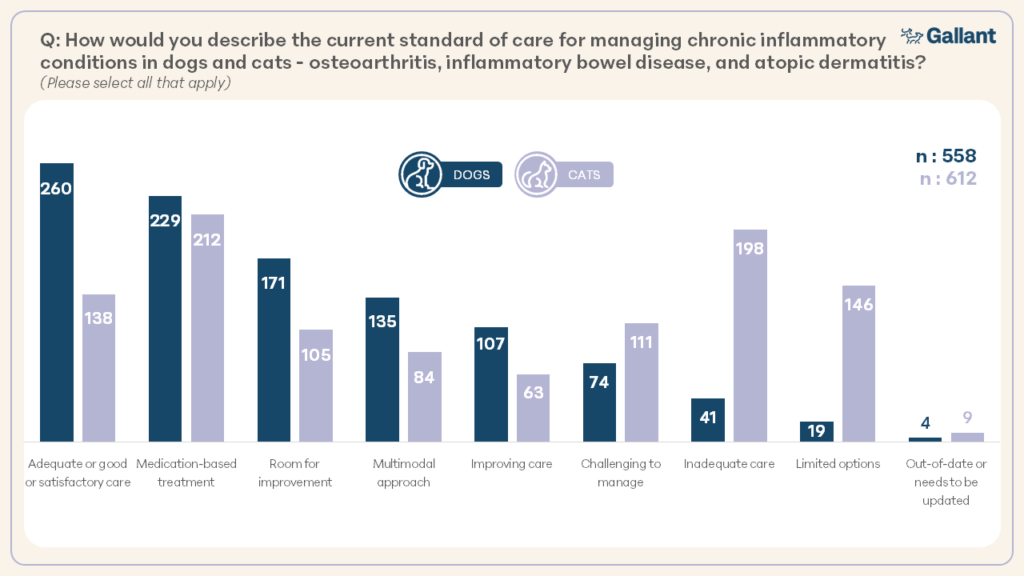
Familiarity with Regenerative Medicine
To assess baseline knowledge, participants were asked how familiar they were with regenerative therapies currently used in veterinary medicine. 10.0% described themselves as very familiar, 58.8% reported being somewhat familiar, and 31.2% indicated they were not familiar at all.
Among those who indicated at least some familiarity with regenerative therapies, 86.7% reported familiarity with platelet-rich plasma (PRP), followed by hyaluronic acid (66.2%), and autologous stem cell therapy (61.2%). Fewer participants reported familiarity with allogeneic stem cell therapy (28.6%), autologous conditioned serum (ACS) or Interleukin-1 Receptor Antagonist Protein (IRAP) (21.8%), or amniotic and placental-derived products (12.7%).
Respondents who selected “Other” referenced a wide range of therapies. These included xenogeneic stem cell therapy, extracellular vesicles and exosomes, autologous serum eye drops for corneal ulcers, along with many others that are not under the regenerative medicine umbrella including monoclonal antibodies, autogenous cancer vaccines, low level laser therapy (LLLT)/photobiomodulation, hyperbaric oxygen therapy (HBOT), Synovetin, and polyacrylamide gels (Arthramid), nutraceuticals, and joint supplements. A few responses reflected limited use (e.g., in ophthalmology) and general awareness without direct experience.
Discussing Regenerative Medicine with Clients
When asked about their confidence in discussing regenerative therapies with pet parents, 65.3% of those familiar with regenerative therapies reported minimal to no confidence. Among those who were not fully confident, the most common reason was lack of adequate training or education in veterinarians (79.8%) (Figure 4) and veterinary technicians (83.4%).
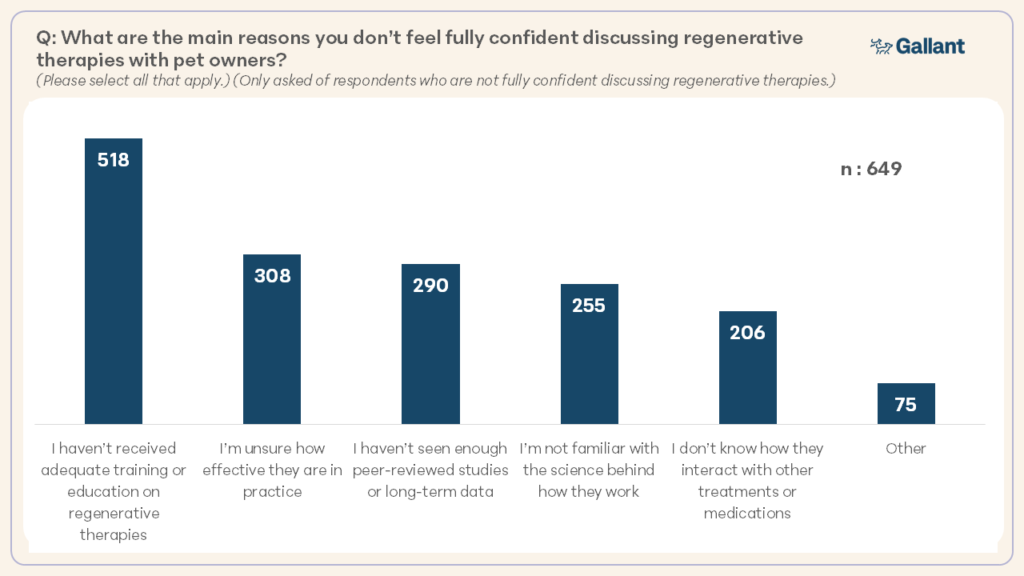
When veterinary technicians were asked what would help them feel more confident supporting regenerative therapies, they reported the need for continuing education, training on how therapies work, and client-facing materials, such as handouts and visuals. Many also noted the value of step-by-step administration protocols, guidance for answering client questions, and access to case studies or success stories.
Pet Parent Interest in Regenerative Medicine
When asked whether pet parents had ever shown interest in regenerative therapies, 43% reported pet parents had either inquired about specific treatments or expressed general interest in regenerative therapies; 53.8% respondents had not received any questions from clients.
Use of Regenerative Therapies in Veterinary Practice
To better understand how regenerative therapies are currently applied in clinical settings, respondents were asked about their use and perceptions of regenerative therapies over the previous 12 months.
Experience with Specific Regenerative Applications
45.3% respondents indicated that they had administered or recommended regenerative therapies for canine patients during the previous 12 months, while only 13.9% veterinarians reported use in feline patients.
Autologous Therapies
The most used autologous treatments from 169 and 76 respondents discussing canine and feline use respectively were: PRP (76.9% in dogs, 66.7% in cats), autologous stem cell therapy (41.4% in dogs and 52.9% in cats), and ACS/IRAP (18.3% in dogs and 13.7% in cats). Respondents also reported using other autologous products including serum eye drops, topical ophthalmic products for corneal ulcers or abrasions, and autologous protein solution (APS).
Allogeneic Therapies
Reported use of allogeneic therapies included allogeneic PRP (43.4% in dogs, 25% in cats), off-the-shelf stem cell therapy (34.2% in dogs, 53.6% in cats), and amniotic or placental-derived products (31.6% in dogs, 35.7% in cats). The relatively high reported use of “off-the-shelf stem cell therapy” may reflect respondent confusion of this category. Free-text responses suggest that some clinicians included non–off-the-shelf, non-regenerative therapies including monoclonal antibodies, shockwave therapy, donor serum products, or combination treatments under this category, which may have inflated reported usage.
Veterinarian Satisfaction with Regenerative Therapies
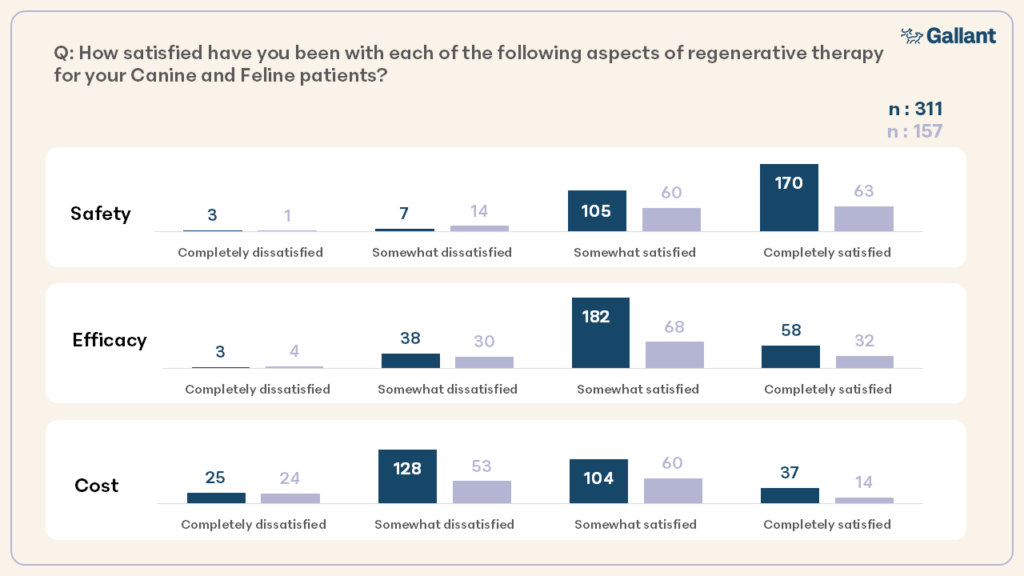
96.4% and 89.2% of veterinarians who had administered regenerative therapies for canine and feline patients respectively reported satisfaction with safety (mean satisfaction 3.55/4 in dog and 2.99/4 in cat). 85.4% and 74.6% for canine and feline patients respectively reported satisfaction with efficacy (mean satisfaction 3.05/4 in dog and 2.96/4 in cat). 48.0% and 49% for canine and feline patients respectively reported satisfaction with cost (mean satisfaction 2.52/4 in the dog and 2.95/4 in the cat) (Figure 5).
Comparison to Other Therapies
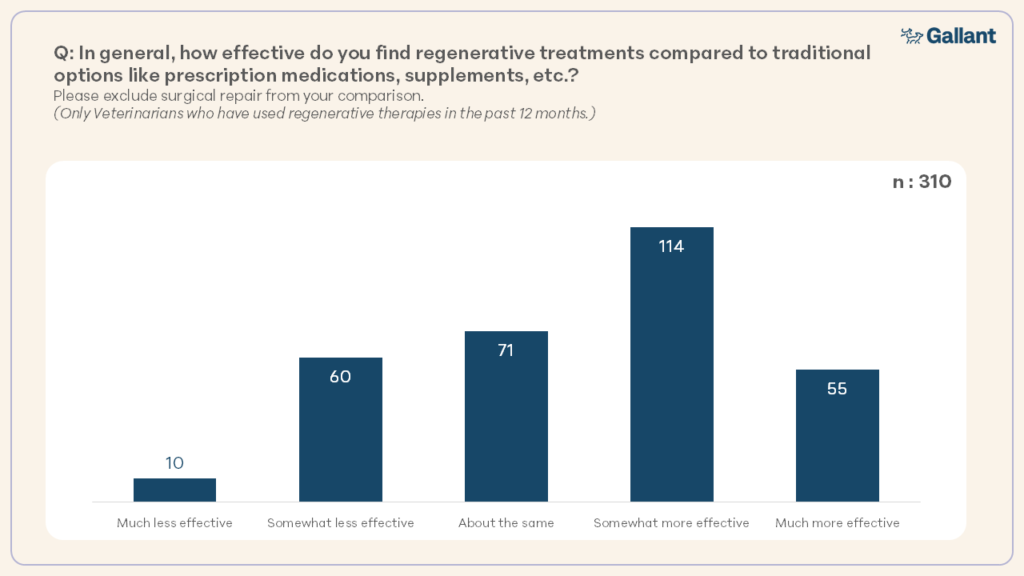
54.0% of respondents who had used regenerative therapies in the prior 12 months agreed that they are more effective than prescription medications, supplements, and other traditional options (Figure 6).
Allogeneic Stem Cell Therapies in Veterinary Practice
The survey included a focused section on allogeneic (donor-derived, off-the-shelf) stem cell therapies that explored current familiarity, clinical applications, perceived advantages, and any cautiousmess towards this emerging therapeutic option.
Familiarity and Use of Allogeneic Stem Cell Therapies
72.2% of respondents reported no familiarity with allogeneic stem cell therapies, 24.2% were somewhat familiar, and 3.6% were very familiar. A small number of respondents reported using allogeneic stem cell therapies in canine and feline patients for conditions that are part of active stem cell therapy clinical trials including osteoarthritis, post-operative orthopedic recovery, feline chronic gingivostomatitis, wound management, chronic kidney disease, atopic dermatitis, and inflammatory bowel disease.
Perceived Advantages and Concerns Regarding Allogeneic Stem Cell Therapies
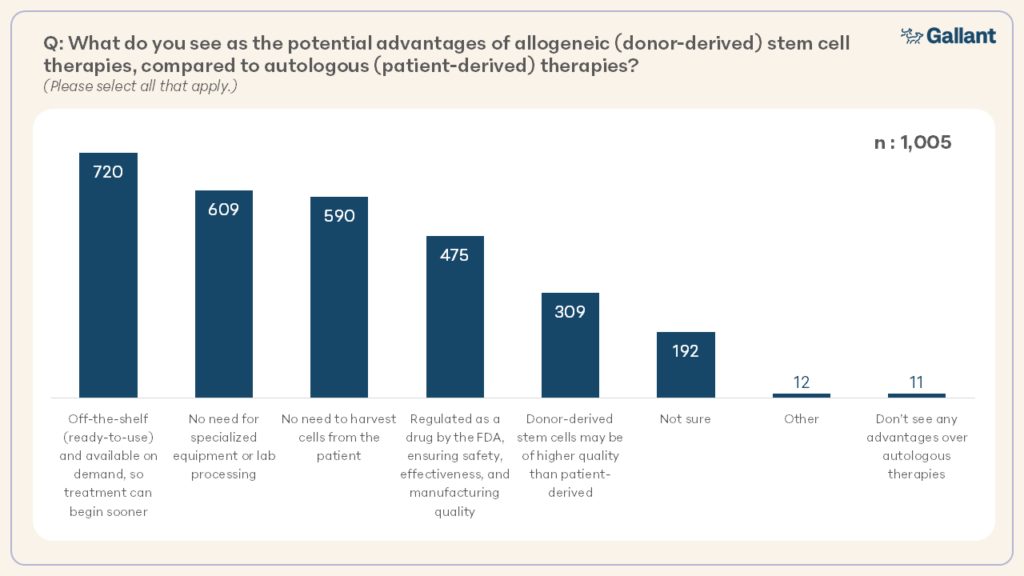
The most widely recognized advantages of allogeneic stem cell therapies were convenience, accessibility, faster treatment initiation, removing the need to harvest cells from the patient, and lack of equipment or lab processing requirements (Figure 7).
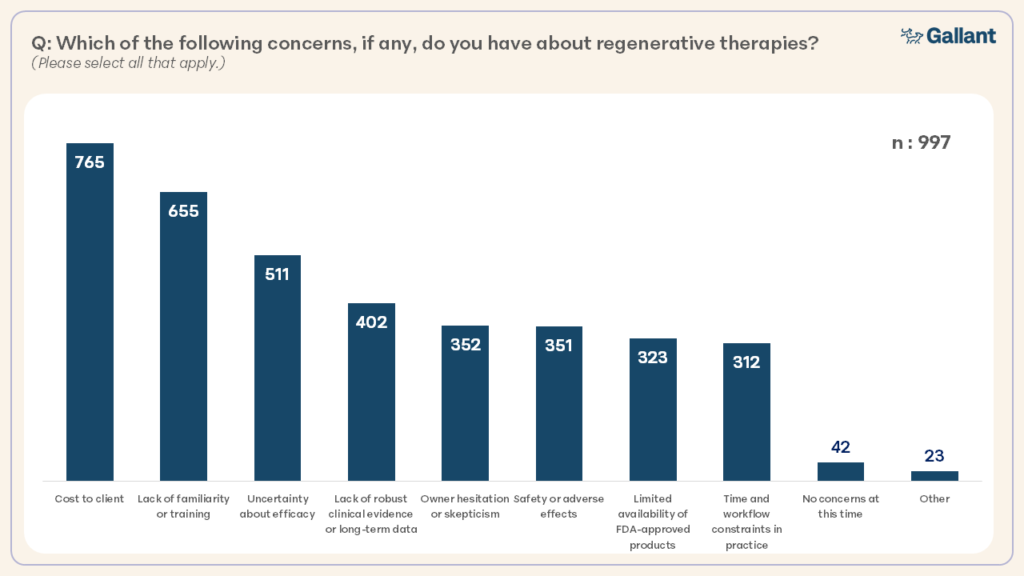
Overall, the most common concerns about regenerative therapies were related to client cost, limited familiarity or training, and uncertainty about efficacy (Figure 9).
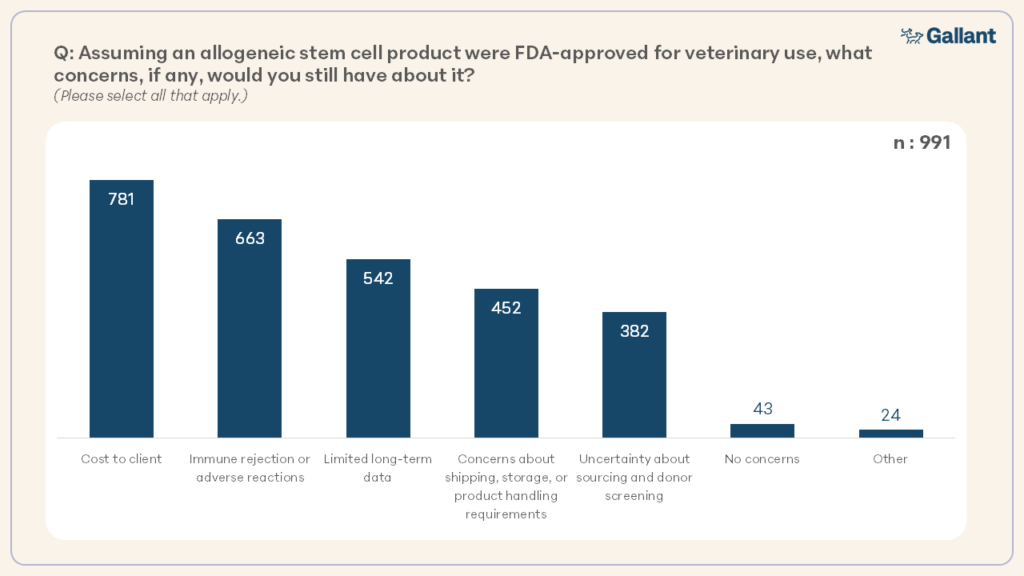
The greatest concerns for a potential FDA-approved allogeneic stem cell product centered around cost, concern for immune rejection or adverse reactions, and perception of limited long-term data (Figure 9).
Regenerative Medicine Referral Patterns
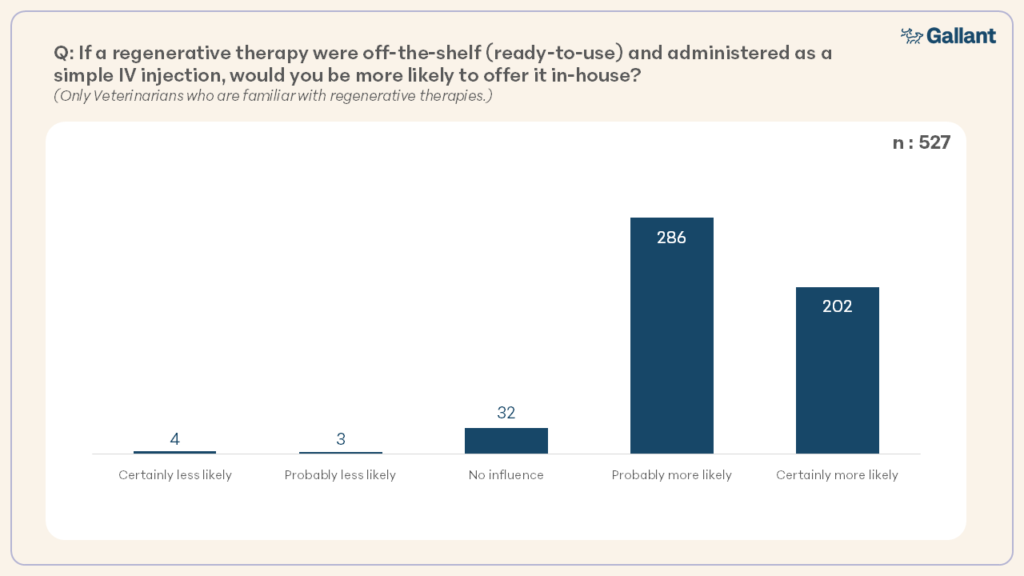
Of 356 respondents currently recommending regenerative medicine, 64.6% refer patients out-of-hospital for therapy. In a larger group of 527 respondents, 92.6% said they would be more likely to offer regenerative therapy in-house if it were off-the-shelf and administered as a simple IV injection, including a large percentage of those not currently offering regenerative therapies (Figure 10).
Anticipated Adoption of Stem Cell Therapies in Veterinary Practice
The final section examined respondents’ expectations about the future role of stem cell therapy in clinical practice, focusing on the likelihood of adopting or recommending these treatments and the key factors that may drive that decision.
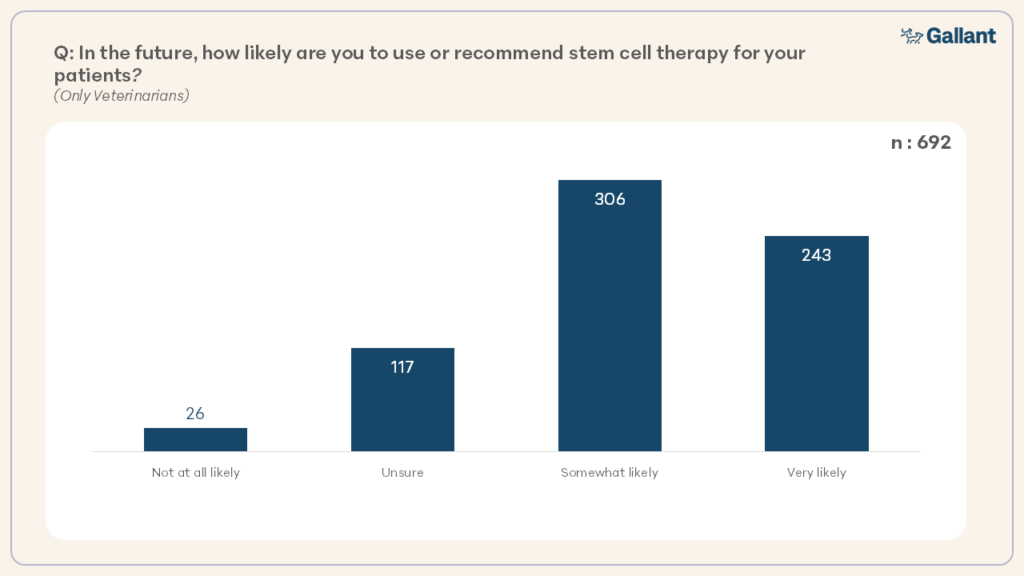
94.5% of respondents believed that regenerative medicine is on track to become a standard treatment option for dogs and/or cats within the next decade. 79.3% of veterinarians were likely to use or recommend stem cell therapy for their patients (Figure 11).
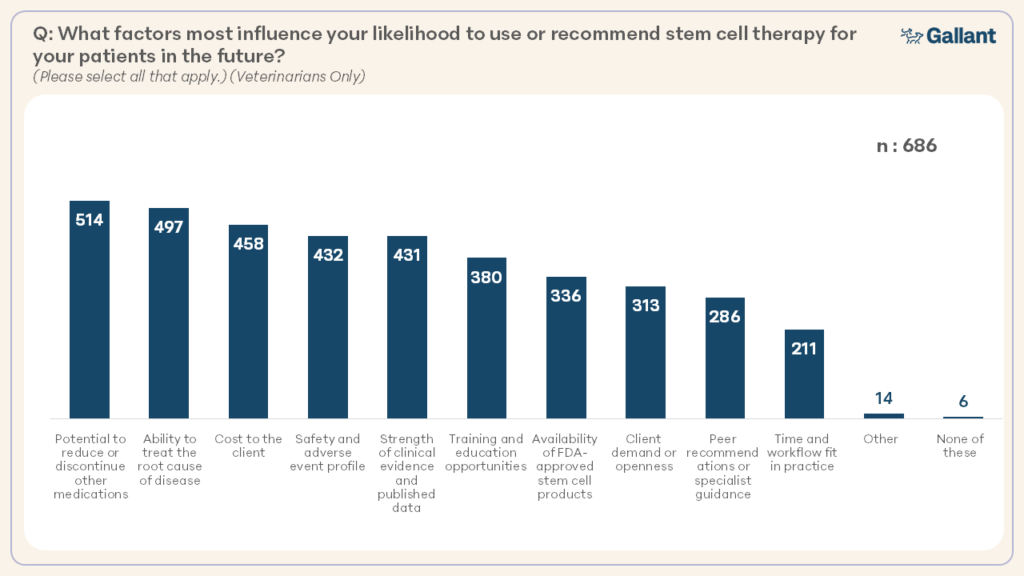
Top motivators influencing future adoption included the potential to reduce or discontinue other medications and the ability to target the root cause of disease (Figure 12). Veterinarians also pointed to client cost, safety profile, and the strength of clinical evidence as key factors shaping their likelihood to use or recommend stem cell therapies.
Summary of Open-Ended Responses
In open-ended responses, many participants expressed optimism about the future of regenerative therapies, noting both their potential and the need to expand access. Common themes included a desire for more education and training, calls for greater standardization and research, and desire for larger, peer-reviewed, comparative clinical studies. Others cited cost as a barrier to client uptake, particularly when treatment benefit, durability, or retreatment intervals were perceived as uncertain. Access constraints were also described, including limitations in rural or resource-limited practice settings and barriers associated with equipment, product availability, or referral logistics. Several responses addressed the need for client-facing materials and communication tools to support informed consent and set expectations. Themes included explaining mechanism of action and realistic outcomes, avoiding overpromising, and supporting adherence to follow-up plans.
Responses showed heterogeneity in perceived effectiveness and readiness to adopt therapies in routine practice. Some entries described strong confidence based on favorable clinical experiences, while others emphasized uncertainty, mixed outcomes, or insufficient evidence to support broader use. Variability was also described in perceived feasibility, including differences in procedural comfort, workflow fit, and the practicality of implementing therapies in clinics with limited case volume or limited access to specialized equipment or referral infrastructure.
Summary
This survey provides a contemporary view of how veterinary professionals perceive regenerative medicine within the context of current clinical practice. Across canine and feline inflammatory conditions, the large majority of respondents (approximately 87%) indicated that currently available therapies primarily manage clinical signs rather than modify underlying disease. Fewer respondents believed existing options consistently address root cause. These findings reinforce a perceived opportunity for disease-modifying approaches in chronic inflammatory care.
Familiarity with regenerative medicine was moderate overall, with most respondents describing themselves as somewhat familiar, but only a small proportion reporting strong familiarity. Awareness was highest for platelet-rich plasma and other autologous therapies. Familiarity with allogeneic, donor-derived stem cell therapies was limited, reflecting the absence of FDA-approved products currently available in veterinary medicine. Survey responses also suggest variability in how regenerative therapies are defined in practice, underscoring the importance of clear education and terminology as the category evolves.
Confidence in discussing regenerative therapies with pet parents was generally low, with lack of training cited as the primary factor. At the same time, 43% of respondents reported that clients have already expressed interest in regenerative medicine. Together, these findings highlight a need for focused educational resources, practical protocols, and client-facing materials to support informed conversations and clinical integration.
Use of regenerative therapies was more common in dogs than in cats over the previous 12 months. Among veterinarians who reported using these therapies, satisfaction with safety was high, and satisfaction with efficacy was generally positive. Cost satisfaction was lower relative to safety and efficacy, reflecting the broader economic considerations that shape treatment decisions in everyday practice.
Operational considerations also influenced adoption patterns. Many respondents currently refer regenerative medicine cases out of hospital. However, 92.6% indicated they would be more likely to offer therapy in-house if it were off-the-shelf and administered as a simple intravenous injection. Convenience, accessibility, and removal of tissue harvest and processing requirements were widely recognized as advantages of donor-derived products. While cost and long-term data were noted as considerations, respondents also identified regulatory oversight, standardization, and manufacturing quality as meaningful attributes of FDA-regulated products.
Looking ahead, nearly all respondents (94.5%) believe regenerative medicine is on track to become a standard treatment option within the next decade, and 79.3% of veterinarians report they are likely to use or recommend stem cell therapy in the future. The strongest motivators influencing adoption include the potential to reduce or discontinue chronic medications and the ability to target underlying disease processes rather than symptoms alone.
Collectively, these findings suggest that the profession is optimistic about the role of regenerative medicine while emphasizing the importance of education, published clinical evidence, operational simplicity, and economic accessibility. As standardized, off-the-shelf stem cell therapies approach regulatory approval, broader adoption will likely depend on continued scientific validation, practical implementation support, and clear communication that aligns innovation with everyday clinical realities.
Conclusion
This survey reflects a profession that recognizes both the limitations of symptom-focused care and the emerging potential of regenerative medicine. Veterinary professionals anticipate a growing role for stem cell therapies in the management of chronic inflammatory disease, particularly as standardized, FDA-regulated products become available.
Broader integration into clinical practice will depend on continued scientific validation, practical education, and delivery models that align with real-world workflow and economic considerations. As regenerative medicine advances, the opportunity lies in pairing innovation with clarity, rigor, and accessible implementation—ensuring that new therapies are introduced thoughtfully and responsibly for the benefit of patients, clients, and the profession.


